Enhancing Peripherally Inserted Central Catheter (PICC) Care with PICCPerfect® Pro: A Quality Initiative in an Iowa Regional Health Center (2023)
by Maria Del Mar Gomez
Abstract:
This article presents the findings of a Quality Initiative conducted at a Regional Health Center in Iowa, focusing on the impact of incorporating the PICCPerfect® Pro compared to the standard of care for Peripherally Inserted Central Catheters (PICCs). This pre-post study involved 15 patient participants receiving care in both inpatient and outpatient settings. The initiative aimed to assess the impact of implementing the PICCPerfect® Pro in terms of care and cleanliness, including dressing integrity, frequency of dressing changes, dislodgement rates, patient comfort, and complications related to catheter securement. The results reveal positive outcomes and increased patient satisfaction using the PICCPerfect® Pro.
Introduction:
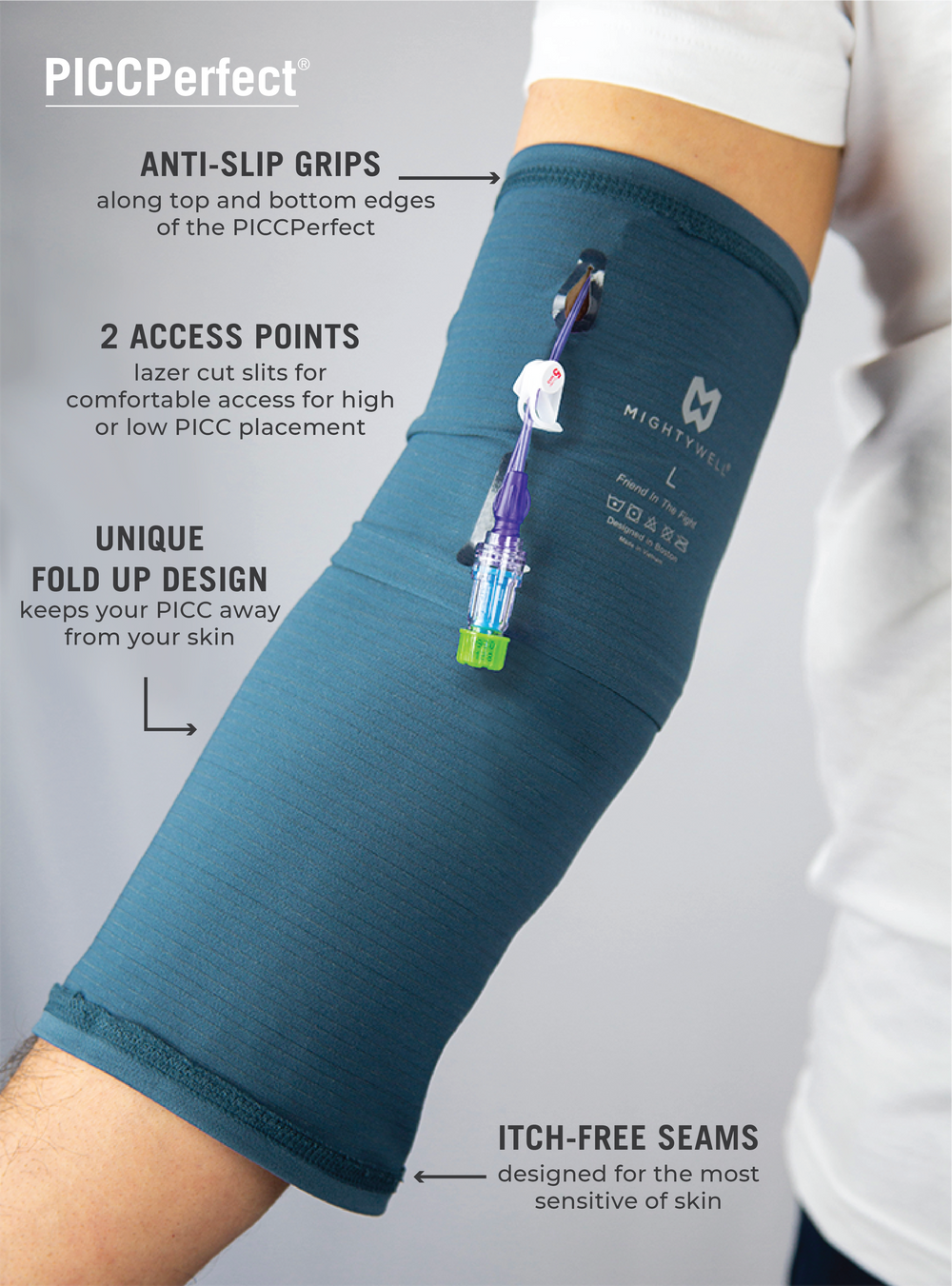
Peripherally Inserted Central Catheters (PICCs) are widely used in clinical settings for various medical treatments. However, dressing integrity and securement can pose challenges, leading to potential complications. The PICCPerfect® Pro is a novel garment-based catheter storage device designed to address these issues and improve the overall experience for patients and healthcare providers.
Methods:
2.1 Study Design:
A pre-post study was conducted to evaluate the impact of the PICCPerfect® Pro on PICC care and patient satisfaction rates when compared to the standard of care for PICCs.
2.2 Participants:
Fifteen patients with PICCs were enrolled in the study, receiving care in both inpatient and outpatient settings. The participants were assigned to the intervention group (using the PICCPerfect® Pro), and the data points were compared against data from the control group (receiving standard of care - uncovered PICC).
2.3 Intervention and Control:
The intervention group had the PICCPerfect® Pro implemented as a garment-based catheter storage device for their PICCs, while the control group had the standard of care, which involved uncovered PICCs with traditional securement methods only.
2.4 Data Collection:
The facility's data was collected and analyzed with the standard of care prior to starting the intervention. Then, the intervention was used, and data was collected for the intervention group. Key variables included monitoring dressing integrity, frequency of dressing changes, dislodgement rates, patient comfort, and complications related to catheter securement.
Results:
The study yielded the following significant results:
3.1 Improved dressing integrity and reduced dressing changes:
In the control group, nurses reported unscheduled dressing changes, rolling dressing edges, and patients picking at dressing, with dressing edges lifting on average on day 3 after dressing placement. Nurses reported enhanced dressing integrity and extended dressing lifespan in the intervention group, which positively impacted patient comfort and decreased nursing workload (Figure 1).
Figure 1. Data pre-post study relating to dislodged catheters, unscheduled dressing changes, PICC failure rates, and patient complaints regarding skin irritation.

3.2 Reduced PICC complications:
In the control group, nurses reported that an average of 10% of their PICCs failed before the intervention, with 5% of these failures being caused by dislodgment. Post-intervention, nurses reported 0% of the PICC failed. (Figure 1).
3.3 Increased patient satisfaction:
In the control group, nurses reported an average of 50% of patients complained about discomfort around skin irritation when their catheter was against their skin (Figure 1). Nurses reported that this data point was reduced to zero in the intervention group, and all participants expressed increased user satisfaction with the PICCPerfect® Pro and its performance. As a result, the facility’s materials management reached out to purchase additional PICCPerfect® Pro for continued use.
Conclusion:
This Quality Initiative demonstrates the benefits of incorporating the PICCPerfect® Pro within the care and maintenance standard for PICCs. The study findings reveal improved dressing integrity, reduced dressing changes, and enhanced patient comfort and satisfaction. The PICCPerfect® Pro effectively addresses common challenges associated with PICC care, leading to positive outcomes for both patients and healthcare providers. Implementing this innovative device can contribute to enhanced vascular access care and improve overall patient experience in clinical settings.
Future Implications:
This study's positive results suggest that PICCPerfect® Pro should be further researched and implemented in larger clinical settings. The device's ability to reduce dressing changes and promote patient comfort has the potential to streamline healthcare processes and improve the quality of care for patients requiring PICCs.












Leave a comment